Become the Sherlock Holmes of health
Back in 2001 when I was a fresh-faced graduate and naive beyond belief, I was all about the magic happening with my hands.
If I could just get better an adjusting and doing SOT techniques, then lepers would be cured and people would rise out of their wheelchairs.
The history taking was really an irritation but done to make sure they didn’t have something nasty like cancer.
The non-neuromechanical symptoms and family history…..yeah I took it but more out of well drilled college habit and to please the GCC, than from a real usefulness point of view.
The “lens” through which I viewed my patients was a neuro-mechanical one.
Then as my functional medicine knowledge began to grow, the previously inconsequential information, suddenly started to take on meaning.
They were clues to perhaps a bigger health picture and contributors to the “why”.
Why had that nerve pain from the disc injury never fully healed?
Why had they suddenly started getting migraines as an adult?
Diagnosing the pain generator or the pattern you look for with your chosen technique is a great place to start, but it shouldn’t necessarily be the end of the detective work.
The more chronic they are, the more you need to dig deep and look for the underlying why.
You need to become a Sherlock Holmes like detective and look for the clues to why they are in your clinic.
Detective work actually runs in the family, my daughter started “The daring detectives” with a school friend as you can see, they provide a comprehensive service at competitive rates.


These days I let the ACN health questionnaire do the hard work by screening for metabolic dysfunction that could stop my neuro-mechanical care creating significant and sustainable results.

Plus it digs deep into the family history to look for genetic traits that could be evolving into symptoms and as yet undiagnosed “diseases”.
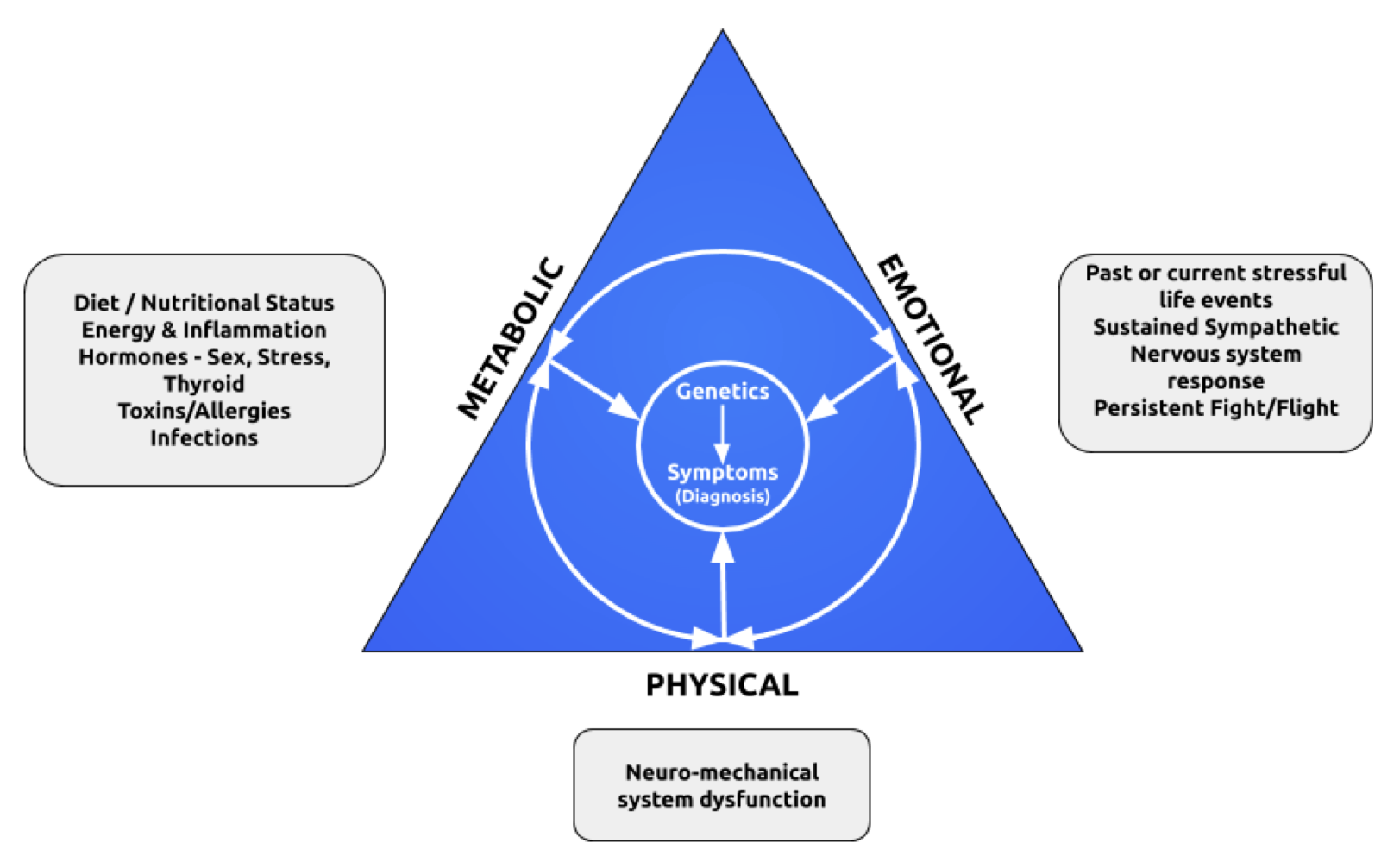
Ultimately we are neuro-mechanical specialists but the body also has metabolic and emotional sides that all come together as one integrated system.
These inputs are filtered through our genes and the outcomes, become our symptoms.
If the patient has persistent pain and tingling despite the best attempts of the local physio, Osteopath or Chiro, plus digestive symptoms.
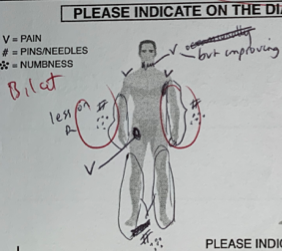
You need to know that a close relative receives B12 injections, or you will miss the diagnosis of subclinical B12 deficiency, which looks “normal” according to the GP.

It is worth noting that the NICE guidance on B12 is clear that the B12 test is not reliable to definitively rule out deficiency and that a grey zone exists above “normal” levels.
Thus:

AKA: If you (and the GP) miss it, they could have a permanent neurological impairment and that is simply not good enough.
ACTION TO TAKE
– Dig deep at the initial consultation and really understand their family history, modify your health questionnaire to do the screening and pick out the detail verbally.
– On Monday 14th September at 8.30, I will discuss vitamin B12 live with the Lions of Chiropractic, you can sign up here
https://www.
or find them on facebook
– Never hire my daughter for detective work, she is a terrible gossip.
